Editorial: Predicting the COVID-19 vaccine
The ISD Editorial Board examines how a COVID-19 vaccine will develop and explores various issues associated with distributing a vaccine.
October 4, 2020
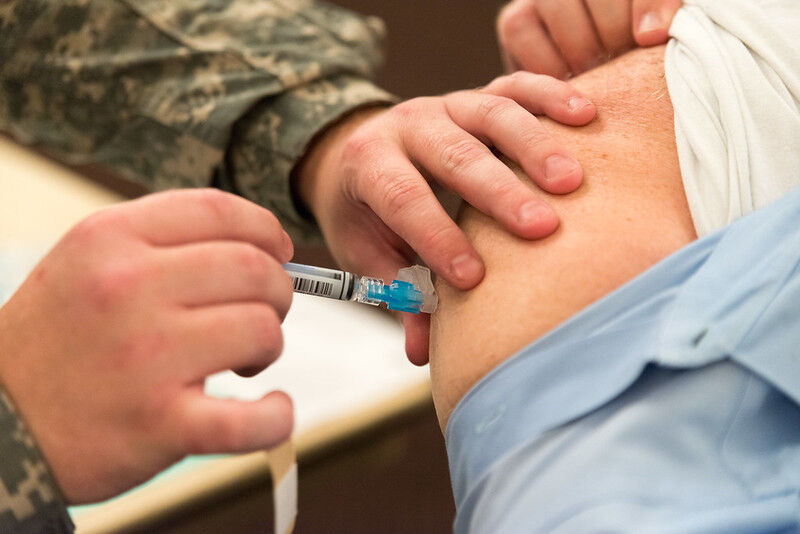
For the majority of the U.S. population, a COVID-19 vaccine marks the return of social gatherings without face masks or constant paranoia. A life with hugging friends and having parties with food and drinks and games, celebrating holidays and birthdays without the 6-foot reminder of the pandemic. Loved ones, canceled plans and missed opportunities are the only thing a vaccine is unable to return.
However, there is still a long way to go before a vaccine is approved through all trial stages, produced in mass quantities, sold or subsidized to the public and distributed effectively. Not to mention the policies that govern every step in the process, including cost, requirements (and exceptions) and distribution.
The U.S. has approved three vaccines to undergo stage three clinical trials with funding from Operation Warp Speed, but there are several dozen other vaccines being tested as well. Meanwhile, in Moscow, a vaccine has been developed and approved by the Russian government, despite incomplete testing and trials.
Many people are worried that in the rush to develop a vaccine, possible side effects may be overlooked or effectiveness may be compromised. While these reservations are completely valid, since most vaccines take years to develop, Andrew Ward, the senior author of one vaccine trial said, “Our findings suggest that the speedy design and manufacture of this vaccine did not compromise the quality of the spike protein structure.”
In order for the vaccine to be effective, the public will have to trust not only science, but the scientists and researchers responsible for prioritizing health and safety. While doubts are understandable, failing to trust the science behind vaccines will only continue to allow COVID-19 to infect more people, ruining more lives and delaying the return of our normal.
There is a danger in politicizing the vaccine, however, which may cause individuals to base their judgements of the vaccine on politicians’ words and actions instead of medical experts and science. Government officials have no authority or place to sway the public’s opinions about vaccines unless they are actively researching and developing a vaccine themselves (which is unlikely).
As for the argument of whether the vaccine should be mandatory, there are already laws and policies in place that govern immunization requirements. In the Jacobson vs. Massachusetts case in 1905, the Supreme Court recognized the necessary protections vaccines provide and, “determine[d] in Jacobson that a state may require vaccination if the board of health deems it necessary for public health or safety.”
In summary, “real liberty for all cannot exist if each individual is allowed to act without regard to the injury that his or her actions might cause others.”
The COVID-19 vaccine would, if deemed necessary by the Board of Health, be mandatory at a state level, which dismissed religious objections “because a compelling state interest may abridge religious freedom.”
Still, people against vaccines may bring up other arguments, such as, “my body, my choice,” which is often used for the topic of abortion. The application of this argument is invalid under the context of a global pandemic; “Abortion is entirely a personal decision that — and this is key — doesn’t affect the health of your neighbor, or your grocery store clerk, or your bus driver. Abortion is not a public health issue, while measles and coronavirus absolutely are. Your body, in other words, is a disease vector.”
Herd immunity, the main goal of vaccines, can only be reached if the vast majority of people get the vaccine. Antivaxxers pose a threat to herd immunity, which can be exemplified in the regions where the measles has recently surged in the U.S.
Possibly the most difficult aspect of the vaccine is effective distribution. Fortunately, there is already a plan in place for who will receive the vaccine first, including health care workers, people with underlying conditions and essential workers.
The cost of the vaccine is still unknown, but could be adequately reduced to allow for bulk purchase through the use of price controls, essentially setting a maximum allowed price for the vaccine. However, the U.S., where many vaccine developers are located has stated, “the priority is to get vaccines and therapeutics. Price controls won’t get us there.” This is alarming since the vaccine could be too expensive for many people to purchase, especially if COVID-19 has already negatively impacted their finances or job security.
Government subsidies offer an adequate solution to this problem, which could be offered to people with low incomes and high vulnerability.
The problem we will be faced with last is the physical distribution of the vaccine, since it relies heavily on transportation infrastructure and preparedness. Citizens of the U.S., as well as every other country, depend on quality bulk manufacturing, timely transportation, as well as hospitals and medical institutes with systems in place to administer the vaccine quickly and safely. Inefficiencies within these processes will have major impacts in the delivery of vaccines. While citizens should be patient, they should also be able to receive their vaccine with ease.
A vaccine is necessary, but without the collective preparation from manufacturing facilities, transportation infrastructure and medical institutes, we will only be met with delays. On the other side, it is imperative that consumers trust in science and get vaccinated in order to live postpandemic.